
- Pregnancy-related fever requires urgent attention due to risks to fetal development
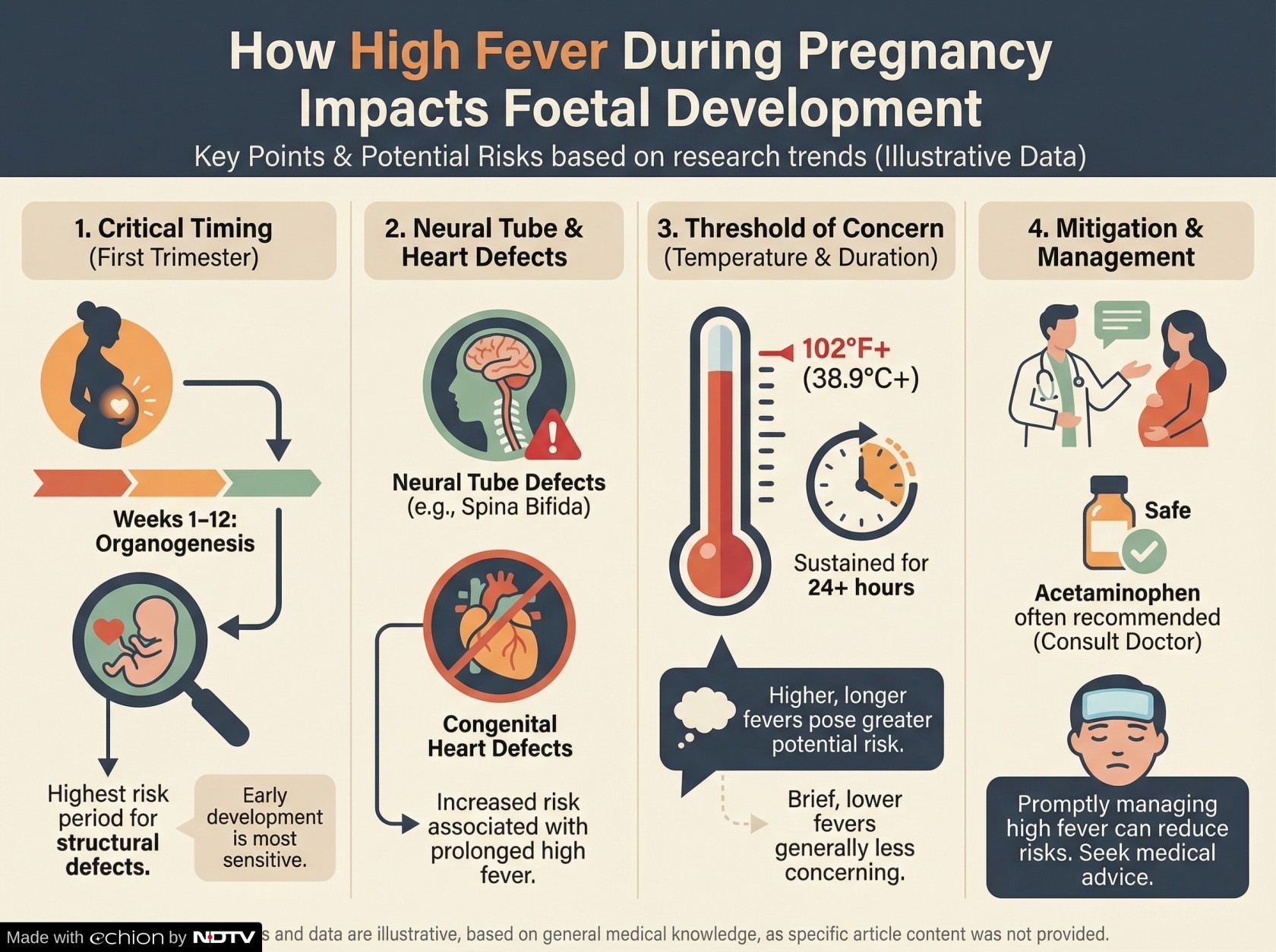
- High fever above 102°F in first trimester may cause neural tube defects like spina bifida
- Fever in later trimesters can affect brain development and increase neurodevelopmental risks
The various physiological changes that occur during pregnancy create a special biological environment, in which even minor changes in the body may have major implications on the developing foetus. In the various concerns that this environment poses, the presence of hyperthermia, as indicated by the manifestation of high fever, is an important clinical variable that needs urgent medical attention.
Even though fever is the body's natural defence against disease, the onset of fever during pregnancy is not just a manifestation of the mother's illness, as it is in the adult, but a form of environmental stressor that may act on the foetus or embryo. An understanding of the mechanisms by which this occurs is crucial for the expectant mother as well as the healthcare provider. The most critical period of risk for fever-related complications is during the first trimester, which is characterized by organogenesis. This is the period in which the basic infrastructure of the heart, brain, and spinal cord of the child is being mapped out in a sophisticated and intricate manner. Research in reproductive biology has demonstrated that the human embryo is highly sensitive to heat. If there is an increase in the maternal core temperature, which is usually defined as an increase of 102-degree F or 38.9 degree C or more, it may affect the protein folding and cellular signalling that is critical in the structural development of the human embryo. In particular, there is an established clinical correlation between high fever in early pregnancy and an increased risk of neural tube defects such as spina bifida. This is because the closure of the neural tube is a temperature-sensitive event, and an increased temperature may result in cellular apoptosis and heat shock proteins that may result in structural irregularities.
After the first trimester, the concerns related to fever are related to functionality and development. In the second and third trimesters, it has been observed that, although the major organs are formed, the development of the brain is in full swing. Prolonged exposure to high temperatures has been observed in the context of neurodevelopmental delays. Some clinical reports indicate that severe inflammatory reactions, usually accompanying fever, are transferred across the placenta. This maternal-foetal inflammatory response has been associated with the central nervous system of the foetus. This in turn has been linked to an increased risk of autism or development coordination problems. Although the risk in any given pregnancy is low, the statistical probability of such occurrences indicates the need for timely regulation of fever.
Additionally, a high fever is rarely an isolated condition; it usually results from an underlying viral or bacterial infection. In pregnancy, infections such as influenza and urinary tract infections can pose significant risks, while chorioamnionitis-an infection of the fetal membranes-represents a serious complication for both mother and fetus. The pregnant woman experiences two different dangers because the fever creates physical stress and the infectious agent threatens her pregnancy. In the later stages of pregnancy, a persistent high fever and the resulting systemic inflammatory response can stimulate the production of prostaglandins. These hormone-like mediators, along with cytokines and reactive oxygen species (ROS), play a key role in activating uterine contractility. This cascade may lead to premature uterine contractions and increase the risk of preterm labour. Thus, what may be a routine, self-limiting illness in a non-pregnant woman can act as a significant trigger for early delivery in pregnancy.
The management of maternal hyperthermia aims at quickly returning the body core temperature to normal to maintain stability in the intrauterine environment. It is generally recommended for the administration of acetaminophen, which is known as Paracetamol, as the first-line antipyretic medication for hyperthermia during pregnancy. It provides complete safety for fever treatment while non-steroidal anti-inflammatory drugs, which include ibuprofen, create potential risks that could harm the developing foetus. The use of non-pharmacologic methods for body temperature reduction, which include lukewarm baths and increased hydration, serves to protect against dehydration because dehydration will lead to higher maternal heart rates and more uterine restlessness. The methods require physician guidance for their proper implementation because only through this method can doctors determine the source of hyperthermia which includes both bacterial and viral origins.
The human body demonstrates extreme resilience, yet the foetal developmental program requires an unchanging environment. A high-grade fever disrupts the body's equilibrium because it creates conditions which can harm foetal development by damaging brain and body cell growth. The primary concern of expectant mothers revolves around identifying problems at an early stage and subsequently informing their doctors about their findings. Early temperature intervention reduces negative impacts on the fetus, which allows the pregnancy to proceed with healthy development.
(Dr Mehnaz Rashid, Consultant - Obstetrician & Gynecologist , Motherhood Hospitals, HRBR Layout, Bengaluru)
Disclaimer: The opinions expressed within this article are the personal opinions of the author. NDTV is not responsible for the accuracy, completeness, suitability, or validity of any information on this article. All information is provided on an as-is basis. The information, facts or opinions appearing in the article do not reflect the views of NDTV and NDTV does not assume any responsibility or liability for the same.
Track Latest News Live on NDTV.com and get news updates from India and around the world



